What is an anal fissure?
Let‘s be frank: anal fissures occur very often. Around 10% of all proctological conditions involve this common tear in the anus, and it mainly affects adults between 30 and 50 years of age. An anal fissure - also known as an anal tear - is a longitudinal tear in the tender, sensitive skin of the anal canal, also known as the anoderm, usually towards the coccyx. This fissure is usually one to three centimetres long and sometimes leads to severe burning or even stabbing pain during a bowel movement. If light red blood on the toilet paper and symptoms such as itching and burning are present, the diagnosis of an anal fissure is confirmed.
Small, but powerful: This small skin defect in the anal canal is anything but banal and can severely impair the quality of life of those affected. The accompanying pain can become so severe that normal everyday life is no longer possible. Due to its severity, a distinction is made between acute (< 6-8 weeks) and chronic anal fissures (> 6-8 weeks) and between primary (without underlying disease) and secondary (with underlying disease) forms. While the chance of healing is very high in the acute anal fissure, the chronic variant can develop skin changes, such as outpost folds, which then make cleaning more difficult. Benign anal fibroma, bulging skin changes or even fistula ducts are also possible. At this point, it becomes really uncomfortable!
In both cases, good anal hygiene is essential to avoid aggravation of the condition through residual stool. The ProctyClean® intimate hygiene pen ensures that the sensitive anal area is gently cleaned, even in places where conventional cleaning methods cannot reach. The wound can heal in peace!
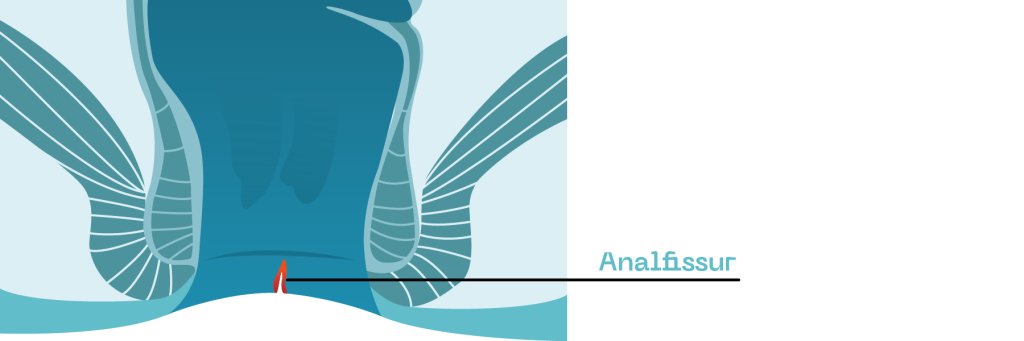
Anal fissures: causes and risk factors
The causes of a primary anal fissure are not yet fully understood. However, fissures often occur in constipation caused by poor eating habits and lack of exercise. As a result, strong pushing during bowel movements is necessary and the tender anal skin can tear.
An anal fissure is not only caused by the large, hardened stool but also by diarrhoea or hemorrhoids. Pregnancies and associated digestive problems are also a possible cause. In addition, infections or inflammation of the rectum (e.g. cryptitis) or a reduced blood circulation of the anal mucosa can be causes. In some cases, well-intentioned anal sex practices during lovemaking can also lead to anal fissures. More rarely, but nevertheless an anal fissure can also occur in the context of certain underlying diseases (e.g. Crohn's disease or HIV). This is termed a secondary anal fissure.
Most scientists agree: an increased muscle tone (= basic tension of a muscle) of the anal sphincter is one of the main causes. This leads to a reduced blood supply to the tissue and to pain and inflammatory stimuli. In order to avoid this pain, an involuntary squeezing posture, which means even more muscle tightening; et voilà - the perfect vicious circle is born!
Anal fissure symptoms: Which symptoms come along with anal fissures?

Quite typical for these small injuries is the combination of the following symptoms: A stabbing, cutting and often violent pain in the anus, which gets worse during and after a bowel movement, combined with a fresh, i.e. bright red bleeding on the stool or toilet paper. The pain may disappear after defecation or instead, leave those affected suffering for hours. Sometimes annoying anal itching may also become noticeable or the wound may show weeping or secretion of mucus.
The stabbing pain results from the tearing of the tender skin and often leads to the retention of stool. But beware: Postponed is not cancelled; the stool continues to thicken, becomes harder, and the next time you go to the toilet it becomes even more painful. The thickened stool also irritates the wound and can also make it deeper. If you are not careful, chronic constipation can result from this holding behaviour. In addition, the sphincter muscle can also cramp due to pain, so that blood circulation is also reduced and healing is less successful. In this case, the conditions are ideal for an acute event to become chronic. If the tear is also deep, there are also morphological changes such as an accumulation and subsequent hardening of connective tissue, so-called outpost folds. These can sometimes even be palpable. In addition, a fissure can also lead to an anal fistula, but this is usually caused by inflammation of the anal glands.
Please do not forget: Blood in the stool can also have other causes, such as hemorrhoids or cancerous diseases, which is why a clarification by a doctor is absolutely necessary, especially in the case of long-term or more frequent bleeding.
Anal fissure diagnosis: Which doctor treats anal fissures and how are they diagnosed?

If an anal fissure does not heal by itself within a few weeks, a doctor should be consulted, no matter how uncomfortable this topic may be to you. If you are embarrassed, you put yourself at risk! The condition can become extremely unpleasant and chronic. Due to the high bacterial count in this area this wound can also lead to serious complications. What doctor treats anal fissures?
Of course, you can contact your family doctor first, but it is even better if you contact a gastroenterologist or proctologist immediately. Procto ... what? Yes, exactly, a proctologist is THE specialist for the rectum and is an expert on the outer and inner life of your butt. And that's why you can put your bum in his/her care with complete peace of mind.
Off the record - what the doctor wants to know from you
Don't worry, the doctor will not get straight to the point. He/She will want to know all of your medical history. This may include questions about the frequency and intensity of the pain or other symptoms such as constipation, itching or possible anal leakage. And after this confidential conversation, it will be a little less uncomfortable to drop your trousers.
Physical examination

After a thorough anamnesis, a careful inspection of the anal region and a possible palpation are performed. This usually takes place on a proctological examination chair or alternatively in a comfortable lateral position. The painful skin defects are also usually found in quite typical positions and usually run up to the rump. The physician speaks of a "6 o'clock position" in a supine position.
If there is an anal fissure, the physician usually finds it here. Sometimes a rectal examination or proctoscopy (endoscopy of the rectum) is still necessary. But don't worry: the proctologist knows exactly how sensitive this sore spot is, which is why it may be suggested to allow a few weeks of healing before further examination. Even then these examinations are usually only performed under local anaesthetic. It is (procto)logical!
Further examinations
If the doctor has not yet found anything definitive or if you have untypical symptoms, further examinations such as smears, biopsies or a rectoscopy may be considered. This could be a colonoscopy, computer tomography (CT) or magnetic resonance imaging (MRI), but also serological and microbial examinations for possible pests from the bacterial or viral kingdom.
Treat anal fissure: What to do in case of anal fissure? What can be done about an anal fissure?
The therapy of an anal fissure depends on its form: Acute or chronic anal fissure, that is the question here! As already mentioned, they differ not only in duration (< or > 6-8 weeks), but also in possible tissue changes. More than 50% of all acute anal fissures experience spontaneous healing and do not require any further therapeutic measures, as the injury is rather superficial. The rest can be treated conservatively, i.e. without surgical intervention; thus 60-90% of all acute anal fissures heal.
In the case of chronic anal fissures, conservative methods and - as a last resort - surgery is also possible. An operation is employed only if all other options have been exhausted. The reason for this is a risk of faecal incontinence - this is extremely unlikely, but who wants that?
Anal fissure ointment

Which ointment for anal fissures? Various ointments and creams are available for the treatment of acute anal fissures. However, please only use them after consulting your doctor! Therapeutic agents like calcium antagonists or nitrates are primarily aimed at reducing pressure in the sphincter muscle. These should be applied several times a day for 3-8 weeks and are recommended as first-line therapy for chronic anal fissures.
Ointments or suppositories with local anaesthetics or cortisone can also be applied to alleviate symptoms. Yes, you read that correctly: This will only relieve the symptoms, but will not affect the healing rate. It is also important to know that their use can also lead to intolerances and (fungal) infections (especially with cortisone preparations). The rule is: as little as possible, as often as necessary!
A good tip: Always wash your hands before applying ointment to prevent wound infections. Also make sure to ensure thorough anal hygiene before applying the soothing cream. The ProctyClean® intimate hygiene pen prevents the treated wound from becoming unnecessarily dirty again by removing residual stool in the terminal canal and the anal folds.
Laxative for anal fissures
Since constipation and the resulting need to squeeze out the excessively hard stool are sometimes the main causes of anal fissures, agents that soften the stool (macrogol, lactulose) and promote defecation are also sometimes helpful. However, these may only be used in consultation with the doctor. General laxatives that empty the entire digestive tract should only be used in exceptional cases as prescribed by the doctor. These disturb natural digestion and often deprive the body of important minerals. In addition, diarrhoea - as we have already heard - can lead to further anal fissures.
Hip bath household remedy for anal fissure

Grandmother already knew: If you are looking for household remedies for an anal fissure, you will find them in a healing bath for the bottom. And rightly so, because hip baths with various additives (mostly from the plant world) ensure better blood circulation, relax the sphincter muscle, support the feeling of hygiene and relieve itching and pain – at least short term. It has been proven that these baths increase the well-being of those affected, but that a higher healing rate is not achieved by soaking the backside. Unfortunately, skin irritations are a common occurrence, which is why one has to be particularly careful when choosing herbs for open skin areas.
Anal hygiene for anal fissures - it‘s the thoroughness that counts!
You can't avoid this: the cornerstone in treating anal fissures is correct anal hygiene. After all, you don't want trillions of germs or irritating substances to be present. Does the thought of toilet paper make you cringe? You are right to feel this way because there is not much you can do with conventional methods using dry toilet paper. However, cleanliness is still necessary! Therefore, the general recommendation is: Please, as often as possible, simply clean the anal area just using lukewarm water. Fragranced cleansers just destroy the important acid mantle of the skin and have no place in open wounds anyway.
One more thing: moist toilet paper (unfortunately also the version for babies) often contains irritating ingredients that sooner or later can lead to allergic reactions. Therefore, please avoid.
Practical - prophylactic - ProctyClean®: Intimate care kit with depth
Have you thoroughly cleaned your bottom with lukewarm water, but hours later you feel wet or a burning sensation again? This may be because your bottom was not quite as clean as you might have thought. When cleaning the anal area, one thing is often forgotten: The cause of the irritation is often still there and is waiting in the anal canal for ideal conditions to emerge. You are supposed to relax the sphincter muscle when having an anal fissure, which is unfortunately not ideal for preventing stool and fluid leakage. In order to prevent this, the sphincter muscle immediately tightens again, and this is the worst thing that can be done for the development of anal fissures.
With the ProctyClean® intimate hygiene pen you clean the source of the problems of irritated and inflamed skin or wounds: the anal canal. To do this, the ergonomically shaped pen is moistened with soothing vitamin E oil and gently inserted into the anus. Ideally, this should be done during the daily shower and according to the slogan "Drilling me softly"! There, ProctyClean reliably removes remaining stool residue from the anal canal and the fine folds of the anus. Thus there is no residue to leak out later. Only this thorough method of hygiene gets your anal area thoroughly clean both inside and out. In this way the wound can heal in peace - without being disturbed by irritating substances.
If the increased hygiene with the ProctyClean® intimate hygiene pen does not improve or if it worsens symptoms, please consult a doctor of your choice!
Nutrition and anal fissure: What should you eat if you have an anal fissure?

As you already know, the right diet plays a crucial role in preventing anal fissures or their recurrence. The stool should be and remain soft, which is why a high-fibre diet is essential. About 30 g of fibre should be consumed per day. These are mainly found in wholemeal products, vegetables and fruit. Also wheat bran or Indian psyllium seeds are true fibre miracles - be creative! But please note: Dietary fibre can only properly bulk and pass through the intestine if there is also adequate fluid intake, otherwise they can even cause constipation. Therefore: Please drink at least 1.5-2 l daily; preferably water or unsweetened herbal teas. You don't like it still? Then of course sparkling mineral water is also an option.
Bad gas: Does all of that healthy food not sit well with you, do you feel bloated or experience embarrassing wind? Then cut back a bit on the dietary fibre until your bowels have adjusted better to it.
Anal fissure stretching - stretching for the buttocks
In the presence of a chronic anal fissure, many proctologists rely on the stretching of the anus; this treatment is performed carefully and several times a day with so-called anal dilators. This application can slightly reduce the increased muscle tone of the sphincter muscle, improve the blood circulation of the skin again and counteract the formation of hardened connective tissue. Many anal dilators are prescribed for use at home and show relatively good results - especially in combination with sphincter-relaxing medication: 60-85 % of patients are cured afterwards.
Anal fissure meets scalpel - When is anal fissure surgery indicated?
In more than 90% of cases, the above mentioned methods lead to healing of the anal fissure, especially in acute forms. If a conservative therapy of more than six to eight weeks is not effective for patients with chronic anal fissure (recurrence rate is often 50%), a surgical method can be considered. At the patient's request or, for example, in the presence of fistulas or pronounced morphological changes, an operation may be recommended immediately.
For this purpose, a so-called fissurectomy is performed, in which the tear is cut out. This also eliminates any possibility of pocket and niche formation and scarred tissue (e.g. outpost fold) is removed. This creates an open wound, which must be kept clean for a few weeks by showering until it heals. To ensure that all anal fistulas can be removed at the same time, this procedure is always performed under anaesthetic. Botox can also be used during this procedure.
A method often used in the past, namely the cutting of the sphincter muscle (sphincterotomy), is no longer used today due to the relatively high risk of incontinence.
Anal fissure: healing process - these are the prospects
As already mentioned, an acute anal fissure usually heals spontaneously and without problems within a few weeks with conservative treatment methods. It is critical to keep the area clean, so that germs or substances from possible stool residue do not aggravate the situation.
If left untreated, there is also the risk that the acute anal fissure becomes chronic and that it will give rise to anal fistulas or abscesses. A chronic anal fissure should therefore be treated surgically after unsuccessful conservative therapy attempts to put an end to this annoying condition.
Whether acute or chronic - an anal fissure can occur again and again if the causes and risk factors are not addressed. Are you ready for changes in your lifestyle?
How can you prevent an anal fissure?

There are some things you can do to prevent a new anal fissure or to avoid ever having one in the first place. One of the most important things is to ensure better stool consistency. Anal fissures are more often than not caused by hard stool or constipation, which is why adequate fibre consumption is necessary. At the same time, adequate fluids must also be consumed in order to properly prepare the fibre or else all of the effort is wasted. Correct bowel movement must be learned: Please make sure that you have regular bowel movements and do not hold back your stool; the large intestine then removes even more water from the stool and this leads to further hardening.
Another point on your to-do list should be exercise. A regular walk, cycling or Nordic walking are all you need, but of course, you can always do a bit more.
ProctyClean® intimate care kit - nice inside and out
Last but not least, if you have an anal fissure, optimal anal hygiene should also be integrated into your everyday life. The patented ProctyClean® intimate hygiene pen gets to the root of the problem and removes the „soil“ at its source before it leaves its mark. This also puts an end to contamination of the wound and possible complication such as common fistulas or abscesses. And there is no fear of injury, because the ergonomically shaped, rounded pen glides particularly gently due to the caring oil and leaves a light and protective lipid film in the anal canal. By the way: Thorough anal hygiene is twice as important for girls due to the anatomical starting point: Who wants to colonize the vaginal area with unpleasant intestinal germs? Targeted anal hygiene - fewer problems!
One thing is for sure: The ProctyClean® intimate hygiene kit is easy to use and time-saving - in just a few minutes your bottom will be spotlessly clean - hygiene with depth. Are you convinced and want to stay clean? Click here to process your order. You will see that prevention is worthwhile!








